Guttate psoriasis is a skin condition that is characterised by the appearance of small red spots on the skin. This article outlines its causes and symptoms and explains the ways in which you can reduce its appearance on your body.
What is Guttate Psoriasis?
Psoriasis is a skin condition that affects between 2-3% of the UK population, or approximately 1.8 million people. Derived from the Greek word ‘psora’, meaning itch, Psoriasis is an autoimmune disease: it causes the body to attack its own cells. This accelerates the natural growth cycle of the body’s skin cells, leading to a rapid build-up of cells that causes scaling on the surface of the skin.
Guttate psoriasis, also known as eruptive psoriasis, is a specific type of psoriasis which causes small, scaly patches that resemble tears or raindrops to appear on the skin (Guttate derives from the Latin, gutta, for ‘a drop’). About 8-10% of those with psoriasis have guttate psoriasis, making it the second most common type of psoriasis after plaque psoriasis.
Guttate psoriasis is a chronic (long-lasting), non-contagious skin condition which is most common amongst children and young adults and is sometimes mistaken for plaque psoriasis. It tends to appear on the limbs and torso, although it can also appear on the face. In the most severe cases, it can have a major impact on the quality of life of those affected; for many, however, it is just a minor irritation, and one that is marked by long periods in which there are no symptoms, or only very mild symptoms.
What causes Guttate Psoriasis
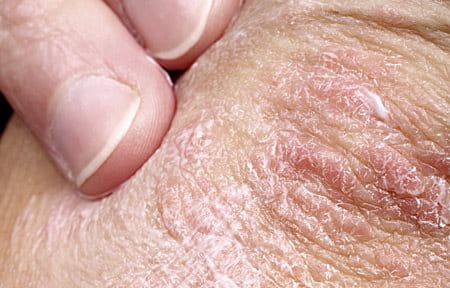
Guttate psoriasis, much like psoriasis in general, is caused by a combination of genetic and environmental factors. It often develops after a streptococcal (bacterial) infection of the throat; the eruption of the lesions on the skin usually happens about two to three weeks after a strep throat infection. It can also be triggered by the following:
- An upper respiratory tract viral infection
- Injuries to the skin, i.e. cuts, burns and scrapes
- Tonsillitis
- Stress
- Certain medications, e.g. beta-blockers and antimalarial drugs
- Environmental factors, e.g. lack of natural sunlight
Psoriasis occurs when the body, mistaking healthy cells for harmful substances, attacks its own cells - which in turn leads to high cell turnover and the formation of scaly patches on the skin.
Doctors believe that this immune response is genetic in nature. This means that the children of those who suffer from guttate psoriasis are more likely to develop this skin condition: in about a third of cases, psoriasis runs in families. The various triggers (strep throat, skin injuries, etc.) often ‘unmask’ guttate psoriasis in people who have a family history for this disease.
With that said, there are ways in which you can reduce the risk of flare-ups.
What are the stages of Guttate Psoriasis
There are three stages of guttate psoriasis:
- Mild: lesions have appeared on up to 3% of the skin
- Moderate: lesions cover between 3%-10% of the skin
- Severe: lesions cover 10% or more of the body; in extreme cases, they can cover the entire body.
It is worth noting that guttate psoriasis can have a serious impact on one’s quality of life even if it is only of mild severity: the hand accounts for approximately 1% of the body’s surface area, and guttate psoriasis on the hands can prove difficult, given that they are used for everyday tasks and are constantly on display.
The symptoms of guttate psoriasis, as we have seen, are drop-shaped, salmon-pink papules that are less than 1cm in size, and these can be a source of discomfort, embarrassment, and even depression: the psychological effects of this condition are well-documented.
The good news is that there are steps that you can take to combat both the immediate symptoms and psychological trauma that can result from persistent flare-ups of guttate psoriasis.
Guttate Psoriasis Treatment
Topical Therapy for Psoriasis
There is no cure for guttate psoriasis, but a range of treatments exist which can improve the symptoms and appearance of psoriatic skin patches.
The most common topical therapies for guttate psoriasis are creams and lotions containing corticosteroids or keratolytic agents. Moisturising products and emollients are used as adjunctive care and are beneficial during the remission and flare-up phase of Psoriasis.
UreaRepair PLUS 10% Urea Lotion and UreaRepair Plus 5% Urea Replenishing Body Wash are both suitable for the treatment of guttate psoriasis, and can provide effective relief for the symptoms of this skin condition.
Topical treatments and keratolytic agents are essential for the treatment of psoriasis. They support the efficacy of any systemic drug therapy. During the initial keratotic phase (the name given to the phase when psoriatic plaques start to form), Keratolytic agents are most beneficial due to their exfoliating properties. They help to reduce the scales of psoriatic plaques, as they exfoliate excessive skin. These agents can be used in conjunction with moisturisers and emollients.
Topical corticosteroids are effective at all times, but they should not be used continuously for long periods, so doctors often reserve them for flare-up phases. Topical corticosteroids have anti-inflammatory properties, reducing both the rate at which the patches form and the irritation that comes with them. Moderate strength topical corticosteroids are often used for psoriasis on the face, genitals or areas that require stretching or flexing. They are often used in combination with emollients and moisturisers.
Lifestyle Changes That Can Combat Guttate Psoriasis
Given that stress can trigger flare-ups of guttate psoriasis, identifying effective stress relief practices is essential if you are to effectively combat the problem.
Exercising three times a week can boost your mood, reduce skin inflammation and keep your weight at a healthy level, which can help combat the symptoms. Exercise is the perfect example of a healthy means of dealing with stress, whilst drinking and smoking, which are also often used to alleviate stress, will only exacerbate the symptoms of guttate psoriasis.
The National Psoriasis Foundation recommends that people with psoriasis opt for an anti-inflammatory diet that is rich in fruits and vegetables, lean protein, whole grains, and healthy fats. Avoiding foods that promote inflammation, e.g. junk food, red meat and dairy, is good for your overall health and may help you manage your psoriasis symptoms.
We recommend that you see a doctor if you are concerned about your symptoms, and that you book an appointment with a social worker or psychologist if you find that your confidence has suffered as a consequence of suffering from guttate psoriasis.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.