Living with atopic skin can be difficult, and never more so than during an eczema ‘flare-up’ when skin feels itchy and irritated. This article looks at what we mean by a ‘flare-up’ and explains the two distinct phases of atopic skin. It examines what causes eczema to flare-up and makes informed suggestions to help you treat atopic skin when it is at its most irritable.
What is a flare-up?
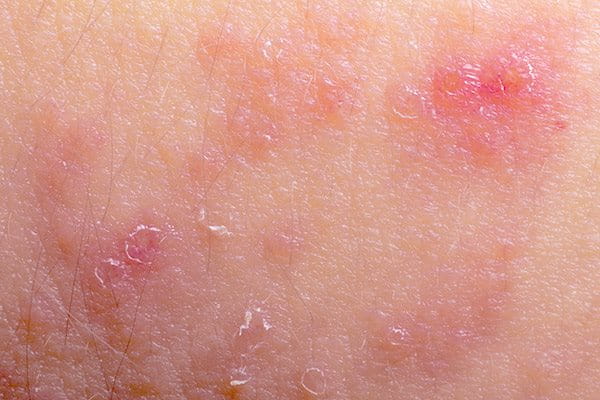
Atopic dermatitis has two distinct phases. A flare-up occurs when skin is at its most irritable. This ‘active phase’ or ‘acute phase’ of the disease includes the following symptoms:
- Itchy or intensely itchy skin. It may be sore too, and some people experience a burning sensation.
- A rash that appears dry, red and flaky. It can be uneven or swollen and may bleed mildly if it’s been scratched.
- Moist or weeping fluid when atopic eczema is very active.
- Small water blisters can develop, especially on the hands and feet.
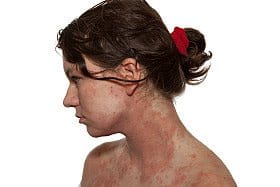
Acute eczema flare-ups can develop anywhere on your body, but the rash is most common on the face, scalp, décolleté/chest and hands. Creases in the joints, like the elbows, knees, wrists and neck, are also commonly affected.
Learn more in Facial Atopic dermatitis, Atopic dermatitis on the head and scalp, Atopic dermatitis on the hands, Atopic dermatitis on different parts of the body, Atopic dermatitis in babies and children and Adult atopic dermatitis.
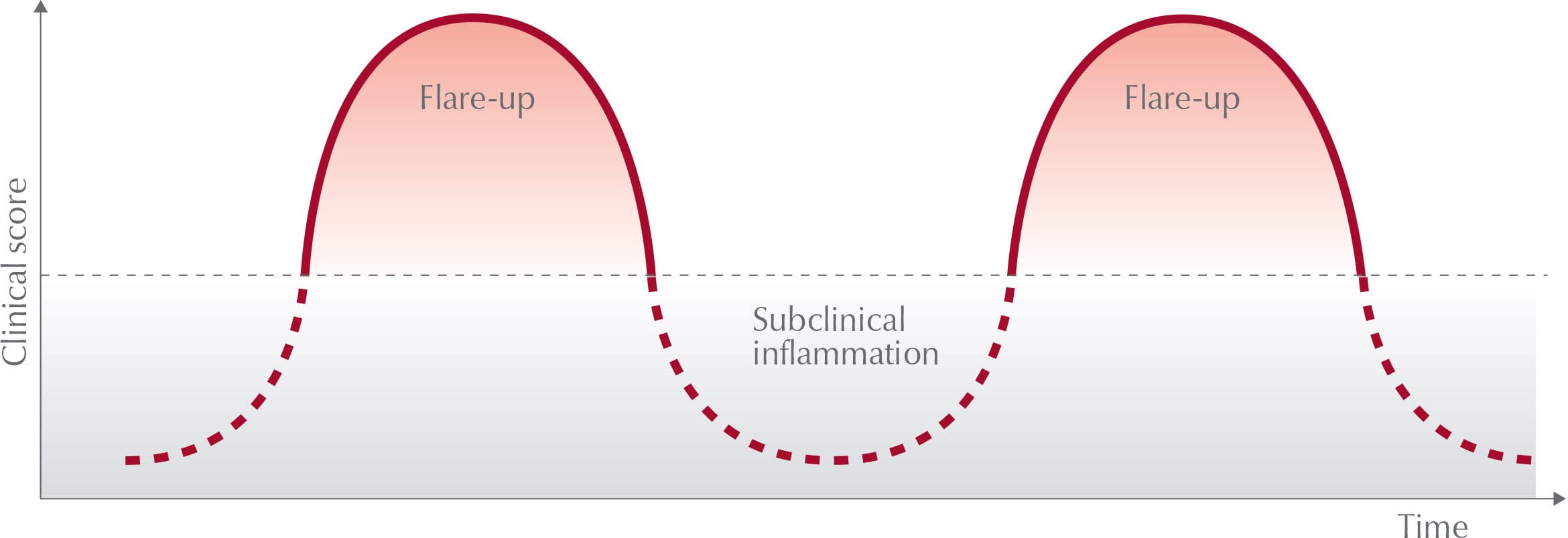
Eczema flare-ups versus non-acute phases
An acute eczema flare-up is by far the most distressing of the two phases and can affect sufferers both physically and psychologically. Eczema flare-ups vary in length from person to person, but thankfully there are steps you can take to soothe skin during a flare-up.
This article explains how you can also reduce the severity of flare-ups and prolong the period between them. Learn more about the period between flare-ups, known as the non-acute phase, in Understanding atopic dermatitis.
How long does eczema last?
For some people, eczema is a chronic condition and flare-ups can take a couple of weeks to subside with treatment. Long-lasting eczema sufferers must take care to avoid triggers in order to prevent flare-ups. However, most eczema sufferers - especially children - will notice their symptoms subsiding with age.
Healing times will ultimately depend on the underlying cause. If a flare-up is caused by a contact eczema trigger, a substance that leads to a flare after coming into contact with your skin, the rash will usually heal within a few weeks after treatment.
What causes eczema to flare-up?
Atopic dermatitis is an inflammatory dry skin disease. Largely genetic, it is linked to a compromised skin barrier function and an immune disorder. Environmental irritants and allergens can trigger a reaction in those already disposed to atopic dermatitis.
As a result of its compromised barrier, atopic skin struggles to retain essential moisture and lipids. It dries out even more and is even less able to protect against external influences. Skin becomes prone to irritation and infection and, because people with atopic skin already have a weakened immune system, they are less able to combat these irritants and more prone to allergic reactions.
Please also note that there are different types of eczema, which can have different causes. By being aware of the type of eczema you have, you can provide the right treatment for it.
Triggers of atopic dermatitis


There are many different factors that can trigger a flare-up and make symptoms worse. These vary from person to person but may include:
Climate and pollution: Changes in temperature, hot and humid climates and the air pollution typical of cities have all been known to exacerbate the condition. Eczema flare-ups are more likely in the winter, with an increase of dry air, indoor heating and hot baths or showers.
Sweat: Sweat can irritate skin’s surface and cause itching and irritation.
Allergies: House mites, pollen and/or dust can all trigger a flare-up. The possible link between diet and eczema is a controversial one, but some people report that certain types of food and drink make their skin worse. The most commonly allergenic foods are eggs, milk, peanuts, wheat, soy, tree nuts, shellfish and fish1,2. Learn more in Understanding atopic dermatitis.
Cigarette smoke: Both smoking and passive smoking can worsen symptoms
Fabrics: Non-breathable fabrics such as nylon, Lycra, polyester and wool can irritate skin. Warm, tight or heavy clothing can make you sweat and cause flare-ups too.
Jewellery: Watches and jewelry often contain nickel. When worn continuously, sweat can oxidise nickel and cause a reaction.
Chemicals: The ingredients in some make-up and sun protection products may trigger a flare-up. Harsh cleansers, some washing detergents and cigarette smoke have also been known to activate atopic skin.
Sun: Some people report that the sun alleviates their symptoms while, for others, it can trigger flare-ups and make skin worse.
Dry skin: Skin can become scaly, rough and cracked when it’s dry, which can then develop into an eczema flare-up if bacteria or allergens enter the skin.
You can find out more about many of these in factors that influence skin.
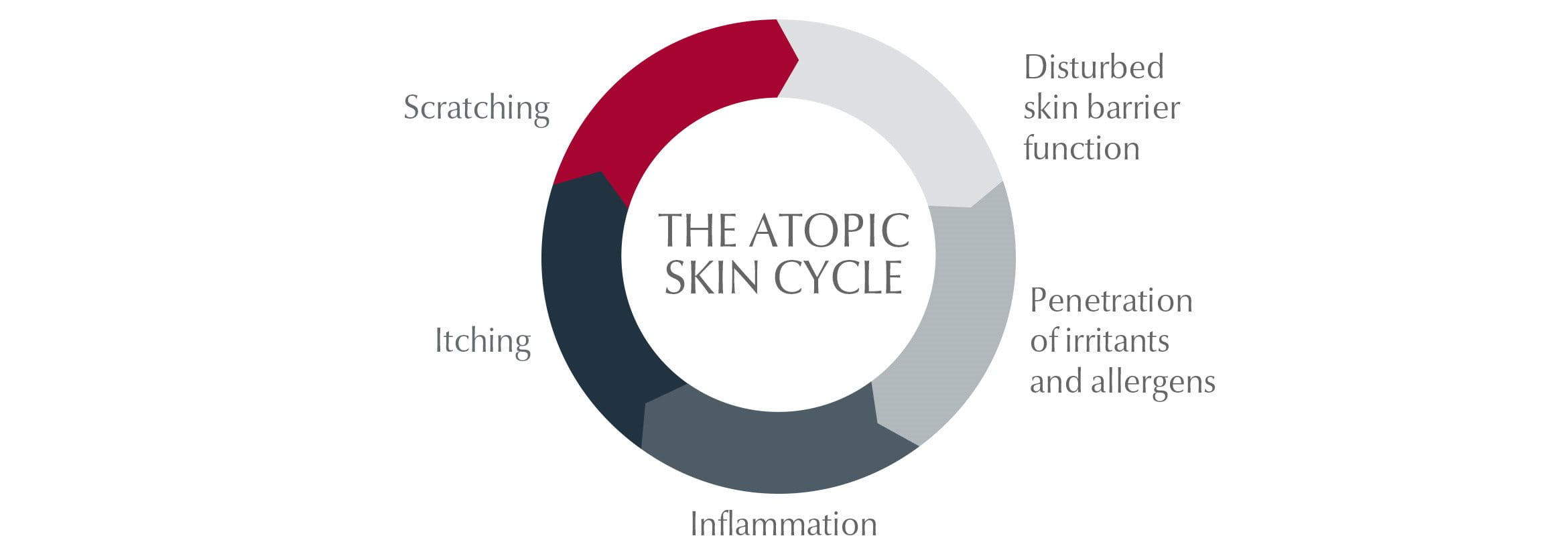
The Atopic Skin Cycle
Symptoms of atopic dermatitis can also trigger and/or exacerbate a flare-up. When skin is dry and itchy, sufferers feel the urge to scratch. This scratching damages the skin's protective barrier and a bacteria known as staphylococcus aureus is able to multiply and infect skin. This infection causes inflammation and itching, which worsens the condition making skin even more irritable and itchy: a vicious circle known as the Atopic Skin Cycle.
Can stress cause eczema?
Yes, emotional stress can trigger an eczema flare-up and affect skin's barrier functions. Our body reacts to stressful situations by increasing the production of stress hormones like cortisol and adrenaline. An overproduction of cortisol can suppress the immune system however, triggering an inflammatory response in the skin. Atopic dermatitis and psoriasis sufferers are particularly susceptible to this inflammatory response.
Stress and eczema can be exacerbated by psychological factors like anxiety, while for some stress may be caused purely by the fact they suffer from eczema, in turn causing a flare-up. Reducing stress in your life won't cure stress eczema completely, but it will help alleviate symptoms and prevent flare-ups. Try the following tips to reduce stress eczema:
- Identify the main triggers of your stress and explore the best way to deal with these in the future
- Exercise regularly and ensure you get fresh air
- Aim to sleep for at least eight hours per night
- Maintain a healthy diet, and drink at least two litres of water each day
- Switch off from your work life and make time to relax, doing things that make you happy
Can a flare-up affect more than just your skin?

Flare-ups of atopic dermatitis can have a considerable impact on quality of life. Beyond the itching and skin discomfort, sufferers report a lack of sleep, discrimination, stress and low self-esteem.
Although eczema is non-contagious, it impacts on family and caregivers too. Relationships are affected by the constant itching, sleepless nights and low self-esteem of the sufferer and, in the case of babies and children, parents often feel guilty and helpless. Read more in How atopic dermatitis affects sleep and quality of life.
How to stop eczema itching
Sadly there is no cure for atopic dermatitis, but there are lots of things you can do to treat atopic skin, calm symptoms and stop eczema itching. For children who suffer from atopic eczema flare-ups, regular use of medical moisturisers can restore the skin's barrier. Treat eczema early, because the more severe the condition becomes, the harder it is to control.
Effective medical treatment and good skincare

Patients who suffer from regular flare-ups will require medical treatment to improve quality of life measures3, so talk to your doctor to find out what treatments would be best for your skin. Options include:
- a steroid, such as Hydrocortisone 1% Cream
- a more potent cream or ointment
- bandages and wet wraps
- phototherapy (ultraviolet light treatment to reduce inflammation)
- oral corticosteroids and, sometimes, antibiotics, to prevent skin from becoming infected
- antihistamines to reduce severe itching
Regular and appropriate skincare can also improve skin condition, support sleep and improve quality of life.4 A non-medical product such as Eucerin AtoControl Acute Care Cream can be used alongside a medical product to soothe skin during an eczema flare-up. Studies show this cream considerably improves sleep and quality of life when used alongside Eucerin AtoControl Lotion.4
Avoid potential eczema triggers
Identifying and avoiding potential triggers is another important step in delaying and reducing symptoms. Speak to your doctor to establish the trigger of your eczema flare-up, so you can try to avoid it. Follow these general tips to prevent flare-ups in the future:
- Do not scratch: Though it can feel tempting and satisfying to scratch affected areas, this can be very damaging to skin and lead to more eczema occurring. Chronic and deep scratching causes bleeding, and increases the risk of scarring or infection. Gently rubbing your skin with your fingers may satisfy the urge.
- Limit scratching damage: Keep your fingernails short and clean to reduce any damage. If your baby has atopic dermatitis, try anti-scratch mittens.
- Moisturise your skin: Avoid dry skin, especially in the winter months, by moisturising two or three times a day. The Eucerin UreaRepair range includes the UreaRepair PLUS: 10% Urea Body Lotion for immediate + 48h relief for very dry, rough skin.
- Avoid hot showers and baths: Hot water can dry your skin out, so use lukewarm water instead and try to limit the amount of baths you take. After swimming, rinse off the chlorine and moisturise after drying.
- Pat dry: Rubbing your skin with a towel after bathing may irritate your eczema, so gently pat dry instead.
- Stay hydrated: Aim to drink at least two litres of water per day to ensure you keep your body hydrated.
- Wear soft clothing: Choose soft, fine-weave clothing or natural materials that are gentle on the skin, and avoid fabrics that cause eczema flare-ups.
- Remove dust: Keep your house clean by dusting often.
Sources
- Overview of Atopic Dermatitis, Avena-Woods C, Am J Manag Care, 2017 June, Vol. 23, No. 8, Supplement S115-123
- Handout on health: atopic dermatitis (a type of eczema). National Institute of Arthritis and Musculoskeletal and Skin Diseases website. https://www.niams.nih.gov/Health_Info/Atopic_Dermatitis/. Published July 2016. Accessed April 13, 2017
- Ben-Gashir MA. Relationship between quality of life and disease severity in atopic dermatitis/eczema syndrome during childhood. Curr Opin Allergy Clin Immunol. 2003 Oct; 3(5):369-73
- Eucerin PiU study. Italy. May 2017
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.