Atopic dermatitis is a common skin disease in childhood and affects many adults too. It’s typically associated with dry, red and itchy skin and can have a significant physical and psychological impact on those whose lives it touches. While there is no known cure, effective skincare has been proven to relieve symptoms and keep skin calmer for longer.
This article gives a general introduction to atopic dermatitis, explains what it is and what the symptoms are. Learn about the possible causes and triggers and what products can soothe flare-ups, alleviate symptoms and care for atopic skin on a daily basis.
What is atopic dermatitis?
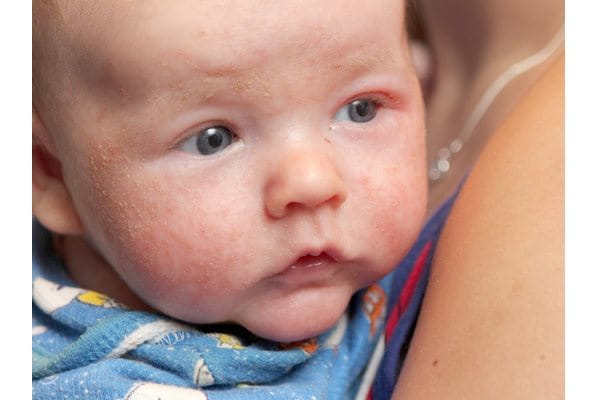
Atopic dermatitis – also known as atopic eczema – is a non-contagious, chronic (i.e. persistent or long-term) inflammatory and non-contagious skin disease characterised by dry, flaky, itchy (also known as pruritic) and irritable skin which can appear on both the face and other parts of the body, such as the legs.
Incidence of atopic dermatitis has increased 2- to 3-fold in industrialised nations since the 1970s. 1,2,3 The disease is increasing in prevalence in developing countries too. Atopic dermatitis is most common in babies and children: approximately 15% to 20% of children globally are thought to suffer with around 90% of all sufferers experiencing symptoms within the first five years of life. 1,2,3
Who is affected by atopic eczema?
It can persist into adulthood and research indicates that those who have atopic dermatitis as children can go on to develop other, related conditions such as asthma and allergic rhinitis4. And, people who never experienced the disease in childhood can also develop it as adults: it is estimated that one in 12 adults suffer from atopic dermatitis 5.
The words are interchangeable and mean the same thing: collective terms for inflammatory changes in the skin. As such, they include many different dermatological diseases. Atopic eczema and atopic dermatitis are also the same thing (atopic means a hereditary sensitivity to certain allergens).
What does eczema look like?
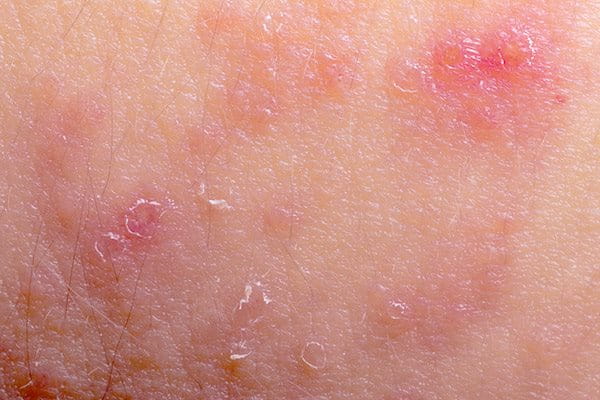
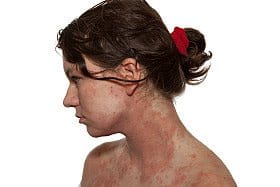
Dryness, itchiness and irritation are all symptoms of atopic skin. In fair-skinned people the affected area of skin is normally reddish in colour and may turn brown. In darker skins, affected skin can become lighter or darker as atopic dermatitis affects pigmentation.
Atopic dermatitis can appear anywhere on the body but the most common locations are: the face (including the area around the eyes), the neck and décolleté, the scalp, elbow folds, knee cavities and hands and feet.
Learn more in Facial atopic dermatitis, Atopic dermatitis on the eyelids, Atopic dermatitis on the scalp, Atopic dermatitis on the hands, Atopic dermatitis on different parts of the body, Atopic dermatitis and babies, Atopic dermatitis and children, and Adult atopic dermatitis.
Eczema flare-ups versus non-acute phases
Atopic skin is typified by two phases:
The acute phase
Atopic dermatitis has two distinct phases. A flare-up occurs when skin is at its most irritable. This ‘active phase’ or ‘acute phase’ of the disease includes the following symptoms:
- Itchy or intensely itchy skin. It may be sore too, and some people experience a burning sensation.
- A rash that appears dry, red and flaky. It can be uneven or swollen and may bleed mildly if it’s been scratched.
- Moist or weeping fluid when atopic eczema is very active.
- Small water blisters can develop, especially on the hands and feet.
Learn more about the triggers of an eczema flare-up, and how to care for atopic skin in Eczema flare-up.
The non-acute phase
Between flare-ups there are periods when atopic skin is calmer and less irritable. This non-acute phase is also known as the non-active, interval or flare-up-free phase.
- Skin feels ‘more normal’ (i.e. the symptoms are less irritating)
- Skin looks and feels dry to very dry and may be scaly, slightly flaky and mildly itchy
- Small, healed cracks (from previous flare-ups) may be visible
- Symptoms are similar to those of dry skin (a condition rather than a disease and known as Xerosis). Read more in Dry skin in general.
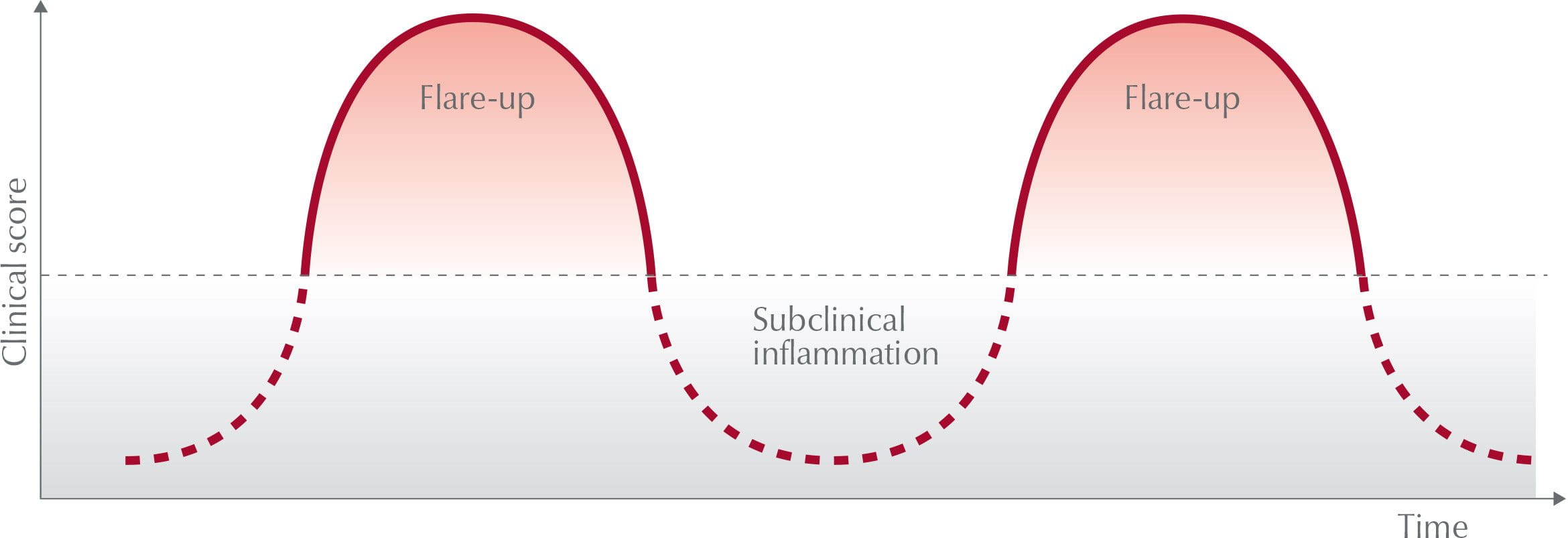
The length of each phase varies greatly on the individual and skincare should be adapted to suit skin’s different needs during each phase.
There is no known cure for atopic dermatitis so the primary aim when caring for atopic skin on a daily basis is to prolong the non-acute phase. During a flare-up, the focus is on soothing symptoms and calming skin as quickly as possible.
For atopic dermatitis treatment, the Eucerin AtoControl range has been specially formulated to give skin the care and comfort it needs during each phase.
How atopic dermatitis affects quality of life
Living with atopic dermatitis, especially during a flare-up, can be distressing and it is known to have a significant impact on quality of life.

In addition to the problems caused by the skin irritation itself, atopic dermatitis can lead to physical and psychological issues such as lack of sleep, discrimination, stress and a general lack of self-confidence.
As a result, sufferers often restrict their daily lives by changing what they wear, what they eat, the make-up they choose and the activities they take part in. Relationships can even be affected if the sufferer feels his or her attractiveness is diminished by their symptoms. And, when it’s babies and children that experience atopic dermatitis, parents can feel helpless and guilty. Stress and eczema are also linked.
What causes eczema?
Atopic dermatitis linked to a compromised skin barrier function and an immune disorder.
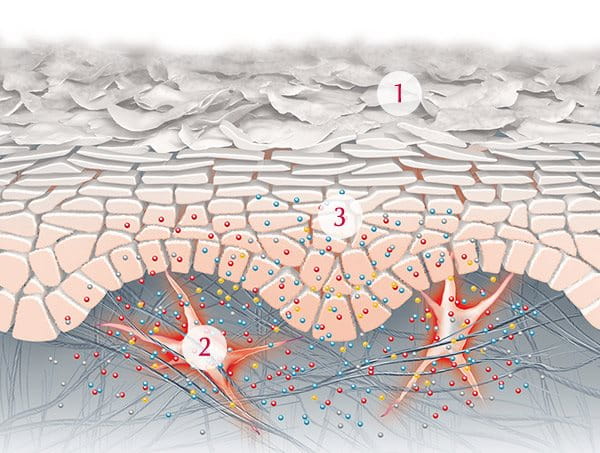
The outermost (epidermal) layers of healthy skin are made up of skin cells (corneocytes) surrounded by a lipid-rich matrix of cholesterol, free fatty acids and ceramide. You can find out more in our Skin structure article. In atopic skin, lipid metabolism is abnormal which causes a deficiency in ceramide and leads to trans epidermal water loss. 4 This excess loss of water causes skin to dry out which weakens its natural barrier function.
The weakened barrier function in atopic skin is also linked to a deficiency of Filaggrin (a gene responsible for the development of structural proteins that strengthen skin’s barrier function). When skin’s natural barrier function is compromised it is more susceptible to irritation and infection.
Sufferers are also known to have an irregular immune function (known as atopy), which makes their skin more reactive to the environment and susceptible to inflammation.
Genetic and environmental theories as to why some people develop atopic dermatitis


Genetic disposition
There are two major risk factors for the development of atopic dermatitis: 1) a genetic defect in the Filaggrin (FLG) gene 1,6 and 2) a family history of atopic disease. 1,3
Children can inherit a Filaggrin deficiency from affected parents 7 and these genetic defects are particularly common among Caucasians.1 Multiple studies have shown that the FLG gene plays a key role in skin barrier function and that mutations of the gene lead to instances of atopic dermatitis. When Filaggrin mutations are present the disease is also more severe and persistent.1
Approximately 70% of all atopic dermatitis patients have a family history of atopic disease.1,3,8 There is a proven link between the atopic diseases: atopic dermatitis, asthma and hay fever. If one or both parents suffer from one of these conditions, there is a chance that their child will develop atopic dermatitis. The risk increases proportionally so if both parents have all three conditions, the chance of the child inheriting the disease goes up.
Climate/pollution
Living in a developed country, a city (especially one with higher levels of pollution) or a cold climate seems to increase the risk of atopic dermatitis.
The Atopic Skin Cycle
Symptoms of atopic dermatitis can also trigger and/or exacerbate a flare-up. When skin is dry and itchy, sufferers feel the urge to scratch. This scratching damages the skin's protective barrier and a bacteria known as staphylococcus aureus is able to multiply and infect skin. This infection causes inflammation and itching, which worsens the condition making skin even more irritable and itchy: a vicious circle known as the Atopic Skin Cycle.
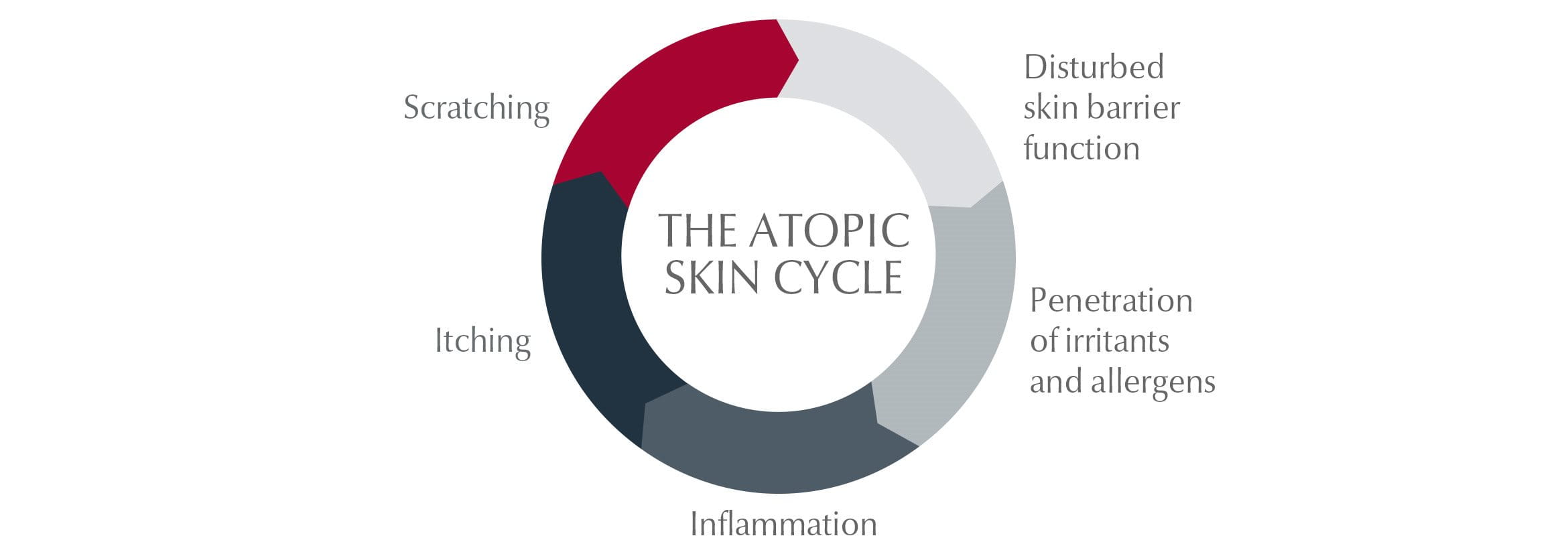
External triggers of eczema


There are a number of external influences that can aggravate atopic dermatitis and make symptoms worse. These vary from person to person but may include:
- climate and pollution
- sweat
- stress
- allergies
- cigarette smoke
- abrasive or non-breathable fabrics: e.g. wool and nylon
- nickel – a metal found in watches and jewellery
- chemicals such as some washing detergents
- sun: some people find that sun triggers symptoms, for others it improves skin condition
You can find out more about many of these in identifying and managing flare-ups and factors that influence skin.
How to treat eczema
A good skincare routine, using products specially formulated for atopic skin, will help to relieve symptoms of atopic dermatitis and to give your skin, or your child’s skin, the best chance of staying calmer for longer.

Effective moisturisation: Key to caring for atopic skin is to restore the skin’s natural protective barrier by giving it the moisturisation it needs. Using moisturisers (also known as emollients) daily helps to prevent or delay flare-ups for as long as possible and is known as basic care. Look out for emollients that include proven actives such as:
- Licochalcone A: An extract of liquorice that soothes skin and reduces redness
- Ceramides: Strengthens the skin’s barrier function
- Omega-3 and Omega-6: Evening Primrose Oil, Grape Seed Oil and Glycine Soja Oil are all rich sources of these essential fatty acids which soothe and nourish skin while replenishing its protective barrier.
The ingredients are part of the active formula in the Eucerin AtoControl range of products that has been specially formulated to care for atopic skin. Emollients can also help to calm skin when it flares-up.
Medicated ointments: Corticosteroids (such as hydrocortisone) can calm atopic skin during a flare-up. Find out more in Identifying and managing flare-ups. Your doctor will be able to advice on the most appropriate treatment for your skin.
Gentle but thorough cleansing: Cleansing is the important first step in caring for atopic skin. Use gentle but effective cleansers that have been specially formulated to be gentle on atopic skin. Try Eucerin AtoControl Bath & Shower Oil for your body.
How to prevent eczema
Because there is no known cure for atopic dermatitis, the best way to care for skin is to do everything you can to reduce the chances of it flaring up. Here are some of the things that others have found can make a difference:
Take care when washing skin: Hot water can dry your skin out, so use lukewarm water instead and try to limit the amount of baths you take. After swimming, rinse off the chlorine and moisturise after drying. Take a quick shower as soon as possible after exercise to cool down your body and remove sweat − heat and sweat can trigger flare-ups for some people. Harsh sponges and massage brushes can also stress atopic skin.
If your work means you need to frequently wash your hands or they are exposed to harsh chemicals then try to limit exposure. You can find out more in atopic dermatitis on the hands.
Keep cool: Keep room temperatures and humidity low and holiday in cool or moderate climates. This will help to reduce sweating which can trigger irritation and itchiness.
Sun protection: Atopic skin is already dry and the sun causes it to dry out further. Limit your exposure, avoid the peak hours when sun is at its most intense, use protective clothing and apply an appropriate sun protection factor. You can read more in the effects of the sun on sensitive skin.
Wear soft, breathable fabrics: Try to avoid harsh and synthetic fabrics next to your skin, as these can cause eczema flare-ups. Opt for fine-weave, soft, clothing or natural materials that are gentle on the skin.
Resist the urge to scratch: Though it can feel tempting and satisfying to scratch your skin, scratching makes matters worse. If you, or your child, is prone to scratching try wearing cotton gloves at night - these can help to reduce damage to the skin.
Make-up: Choose products that have been specially formulated for dry sensitive skin to reduce the chances of irritation.
Try to reduce stress: Relaxation exercises such as yoga and meditation can help reduce stress, which is often cited as a trigger for atopic skin, especially by women.
Diet: We’re all different, but some people find that certain foods and drinks trigger their symptoms and milk, eggs, nuts, shellfish and alcohol are frequently cited. Consider keeping a diary to see if there’s anything that causes your or your child’s skin to flare-up, but don’t make significant dietary changes for babies and children before discussing them with your doctor first. Aim to drink at least two litres of water per day to ensure you keep your body hydrated.
Stop smoking: Cigarette smoke can exacerbate symptoms of atopic dermatitis.
You can find out more about many of these in factors that influence skin.
If symptoms persist, or if your skin or your child’s skin is in any way bothering or concerning you, be sure to contact your doctor.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.