Atopic Dermatitis, also known as Atopic Eczema, is a chronic skin disease which can flare up on the scalp and in the hairline. This article explains how to recognise if you or your child have Atopic Dermatitis as opposed to other common scalp conditions. We look at the possible causes and triggers and make suggestions with regard to caring for atopic skin on the scalp.
How do I know if I have Atopic Dermatitis on my scalp?
If you or your child have red, itchy skin on your head, and if either of you already suffer from Atopic Dermatitis on other areas of the body, it is likely that the symptoms on your scalp are linked. Atopic Dermatitis is especially common in babies and children, but many adults have it too. You can find out more in Atopic Dermatitis and babies, Atopic Dermatitis and children and Atopic Dermatitis and adults.
You should bear in mind that there are several other types of Dermatitis which present similar symptoms and are also common on the scalp. These include:

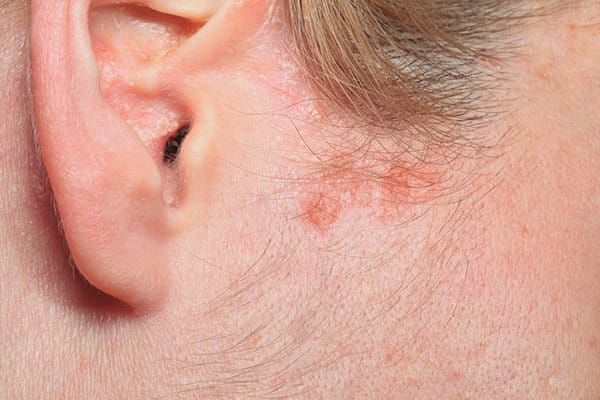
Seborrheic Dermatitis (or Seborrheic Eczema)
A common condition in babies where it is known as ‘Cradle Cap’. Thought by many scientists to be a type of fungal infection (although some believe that it could be genetic and/or linked to the immune system), typical symptoms are thick, crusty, yellowish flakes of skin on the infant’s scalp, although it can also appear on the eyes and nose. Unlike Atopic Dermatitis, however, it is rarely itchy. Most children grow out of it as they get older and are normally symptom-free by the age of three. You can find out more about Seborrheic Dermatitis in general here.
Dandruff
Seborrheic Dermatitis is thought to be one of the main underlying causes of dandruff in adults. There are two different types: greasy dandruff, which manifests as oily, yellowish scales on the scalp, similar to the symptoms of Seborrheic Dermatitis in babies, and dry dandruff, where the flakes are dry, white and loose, falling easily from the head and hair. As with Atopic Dermatitis, the skin often turns red and feels itchy. Dry dandruff is much more common in adults than children, with up to 50% of the adult population suffering from it at some point in their lives. Read more about this subject in Dandruff.
What causes or triggers Atopic Eczema on the scalp?
Psoriasis
Psoriasis, like Atopic Dermatitis, is an inflammatory condition which is likely to have a genetic component. It is also linked to a compromised immune system. Uncommon in babies and children, Psoriasis most commonly affects adults and appears on the scalp. It is distinctive in appearance, with inflamed skin overlaid by silvery scales. In severe cases it can cause hair loss. Find out more in Psoriasis.
Contact Dermatitis:
Contact Dermatitis, also known as Irritant or Allergic Dermatitis, or as Contact Eczema, is caused by the skin reacting to something with which it is, or has been, in contact. Contact Dermatitis on the scalp is caused by a reaction to the chemicals in some shampoos, hair dyes and other hair grooming products. It may be that you are allergic to those ingredients or that they just irritate your skin. Find out more in Contact dermatitis.
Another common cause of itchy scalps in children aged 3-12 years old is head lice. Whilst lice are extremely contagious, they are easy to treat: once they have been diagnosed, your pharmacist will be able to recommend the appropriate treatment. Head lice are normally fairly easy to spot, but do consult your doctor if you are in any doubt.
You can find out more about the symptoms of Atopic Dermatitis, and about how they vary in appearance on different parts of the body, in Facial Atopic Dermatitis, Atopic Dermatitis on the eyelids, Atopic Dermatitis on the hands and Atopic Dermatitis on different parts of the body.
If you are in any doubt as to which condition you have - or if your skin, or your child’s skin, is in any way troubling you - consult your doctor for a diagnosis and for treatment advice.
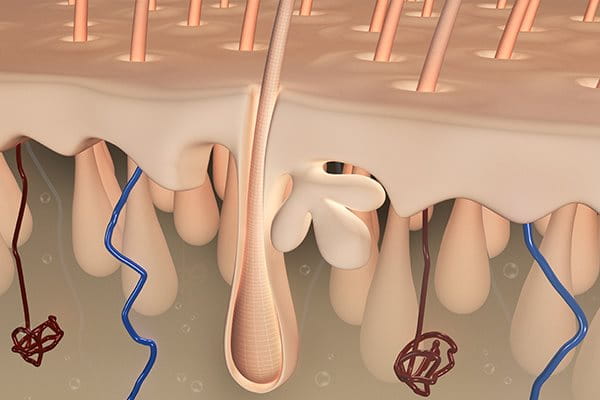
Atopic Dermatitis is a genetic condition that is thought to be linked to a compromised immune system. You can read all about the causes and triggers in Understanding Atopic Dermatitis.
The skin on our heads is significantly thicker than the skin on the rest of the body; it is also densely populated with hair follicles and sebaceous and sweat glands. Our head plays a key role in regulating our body temperature.
Sweat is produced by our skin as a means of cooling itself down when it overheats, and it creates an environment in which the bacteria that trigger and exacerbate Atopic Dermatitis can thrive. Our hair helps to keep this bacteria in place, and the fact that there are numerous follicles means that bacteria has lots of entry points into our skin - as a consequence, atopic skin on our scalp is easily irritated and prone to flare-ups. You can find out more about flare-ups in Identifying and managing flare-ups.
Regular hair-washing and styling can also cause the skin to dry out, further exacerbating the symptoms of Atopic Dermatitis. If your skin is in any way sensitive to the products you use, this can also trigger or increase inflammation. Once the skin has become dry and irritated, scratching it will only make the symptoms worse.
How should I care for atopic skin on the scalp?
For babies with little or no hair, skin care for eczema on the scalp is similar to caring for skin elsewhere on the body. Gentle cleansing and moisturising regularly with products that have been specially formulated for atopic skin, such as those in the Eucerin AtoControl range, will help to give atopic scalps the basic daily care that they need. This will also prolong the period between flare-ups and calm the skin during an acute flare-up. You can find out more in Atopic Dermatitis and babies.
For children and adults, hair can often make caring for an atopic scalp more complicated. Creams and ointments which are easy to apply to other areas of the body can make the hair look greasy and lank, which can result in the person using them feeling depressed about their appearance. Here are some suggestions on how to care for an atopic scalp:


Cleaning your hair and scalp
Wash your hair, and your child’s hair, with a gentle shampoo that is free from perfume and colourants and has been proven to be kind to sensitive skin. Try Eucerin DermoCapillaire Calming 5% Urea Shampoo.
Avoid showering more than once a day, turn down the pressure and use lukewarm water as much as possible. Frequent showering and using water that is too hot can cause further dryness to the skin. A strong blast and cold water can also cause unnecessary irritation to your scalp.
Try not to change products too often, and make sure that you rinse out your shampoo thoroughly. After you have finished showering, wrap a towel around your head to dry it, rather than rubbing your hair dry or using a hair dryer. The rubbing will aggravate your itchy scalp and the heat of the dryer - or other styling products, such as straighteners or tongs - can cause further dryness to your scalp. If you do want to blow-dry your hair, try to use the cool setting and avoid mousses and gels.
Keep your hair and scalp moisturised
Regular moisturisation is important for atopic skin on your scalp. Try Eucerin DermoCapillaire Calming Urea Scalp Leave On Treatment, which is a non-sticky, leave-on formula that delivers hours of intense moisture to your scalp and soothes and reduces itchiness from the first use.
During flare-ups, when soothing and calming atopic skin takes priority over your appearance, you can apply a medical treatment ointment and Eucerin AtoControl Acute Care Cream. Whilst it is not a medical product, nor designed to be used in place of one, Eucerin AtoControl Acute Care Cream is ideal as an adjunctive care product (adjunctive is a medical term, meaning that something increases the benefits of another product). It contains Menthoxypropandiol, an extract of menthol, and Decanediol, an anti-bacterial active - both of which are proven to cool and calm the skin and bring quick relief.
Avoid hair dyes
Try to avoid any products that may dry your scalp out and cause further irritation to your skin.
What else can I do to reduce symptoms of Atopic Dermatitis on my scalp?
Because there is no known cure for Atopic Dermatitis, it is important that you try to identify and avoid potential triggers: this will reduce the chances of it flaring up. You can find out more about the steps that you can take in Understanding Atopic Dermatitis.
If the symptoms persist, or if your skin is in any way bothering you, be sure to contact your doctor.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.