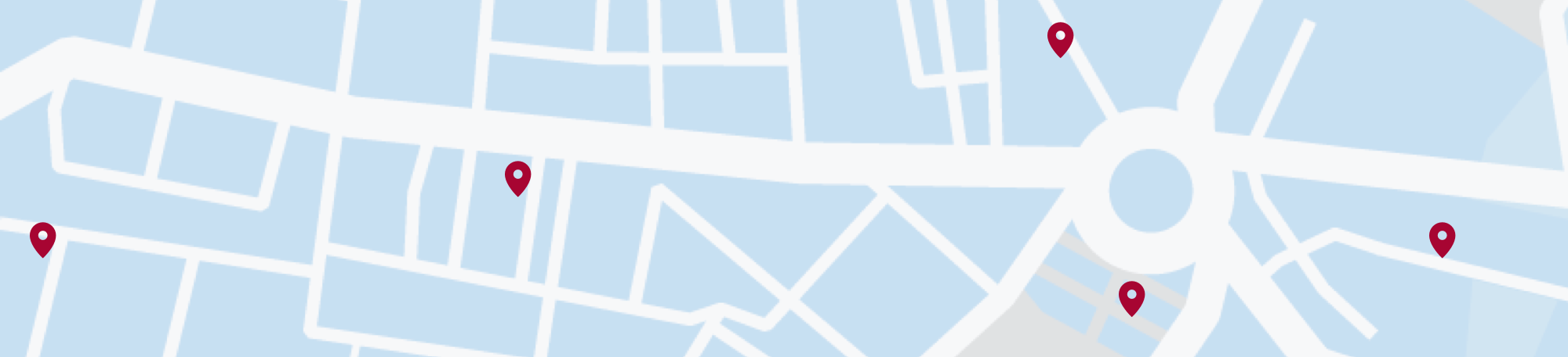
Atopic dermatitis on the hands, also referred to as hand dermatitis or hand eczema, is a common, non-contagious, chronic skin condition. While hand dermatitis is usually a short-term concern, it can affect some people for many years - impacting their daily life. This article explains what to look for, the possible causes and triggers, and makes suggestions on how to care for atopic skin.
What is hand dermatitis?
Hand eczema results in dry, red and itchy skin. Eczema on the hands affects about one in every 20 people1, but the symptoms can vary from person to person. The most severe type of hand eczema is dyshidrotic eczema or pompholyx, where small, itchy blisters develop on the palms of the hands. Contact allergens, as well as genetics, can trigger hand eczema.
(1) British Association of Dermatology, published March 2016Symptoms of eczema on hands
Different parts of the hand can be affected by atopic dermatitis, including the backs of the palms, fingers, finger webs or tips, or in more severe cases of dyshidrotic eczema on the centre of the palms. Eczema on the wrist is also common.
Symptoms of hand eczema can vary from mild dryness, redness and itchiness through to flaking, cracked and intensely itchy hands. This condition has chronic and relapsing phases. Once skin is dry and irritated, scratching makes symptoms worse.
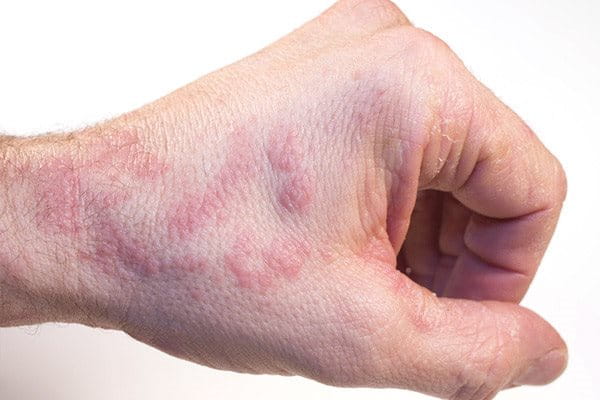
Other symptoms of hand dermatitis include:
- Swelling
- Red or brown plaques
- Skin feeling hot or a burning sensation
- Pain when moving the hand or fingers
- Crusts or pus
In the worst cases skin may develop itchy blisters or cracks, which result in weeping or bleeding.
Who suffers from eczema on hands?
While hand eczema can start during childhood, it is more common in young adult females and working-age adults. Atopic dermatitis on the hands often affects people who work in cleaning, mechanical, catering or hairdressing jobs, or anyone who regularly comes into contact with chemicals and other irritants.
As with all types of atopic dermatitis, hand eczema is non-contagious but it can be difficult to live with and cause problems in the workplace. You can find out more in How atopic dermatitis affects sleep and quality of life.
Mild psoriasis on the hands can also look similar to hand eczema, so if you are in any doubt about your symptoms, you should consult your doctor for an accurate diagnosis. Find out more in our psoriasis article.
If you or your child already experience atopic dermatitis on other areas of your body then it is likely that the two are related. Learn more about this condition on our website:
Causes of eczema on hands
Though the exact cause of atopic dermatitis is unknown, some people have a genetic propensity to atopic dermatitis and you can read about the possible causes of that in Understanding atopic dermatitis. This underlying condition makes them more sensitive to external irritants and allergens and therefore more likely to develop hand eczema.

But people without an underlying condition can also develop hand eczema. The structure of skin on our hands means that it is already more prone to dryness than on other parts of our body. Frequent washing or repeated contact with water (sometimes known as ‘wet work’), cold weather and chemicals in the workplace can all damage the external layers of skin. This causes it to dry out, making it even more prone to irritation. This condition is known as irritant contact dermatitis.
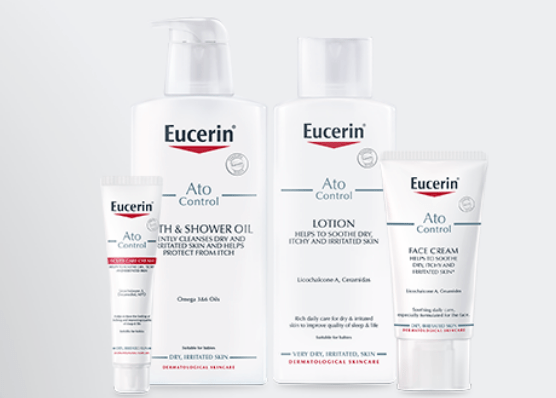
Another form of contact dermatitis, known as allergic contact dermatitis, is much less common and occurs when the body becomes allergic to a substance after regular exposure. Symptoms are similar, as is treatment. Common allergens include hair dye, perfume, nickel (used in jewellery and watches), leather, latex in rubber gloves and certain types of plants. To find out if an allergy is causing allergic contact dermatitis, a patch test can be carried about in a dermatology department.
For many patients, however, the cause of dermatitis on hands is unknown and a trigger cannot be identified. It's also possible for there to be more than one cause of a person's hand eczema, such as a combination of irritant contact dermatitis and atopic dermatitis.
How to treat eczema on hands

While the best treatment for hand eczema is to avoid the triggers that cause it, regular and effective skincare will also help you to give your skin the support it needs. This will help you prolong the periods between flare-ups and soothe skin when it’s at its most irritable and itchy. Be consistent with your daily care routine.
Hand washing
Wash your hands in lukewarm water - avoid temperatures that are too hot or too cold. Use a gentle, fragrance-free handwash or cleanser that has been specially formulated for regular use and/or for atopic skin such as Eucerin AtoControl Bath & Shower Oil.
Try to avoid water-less, antibacterial cleansers as they often contain alcohol and solvents that can exacerbate your symptoms and make flare-ups worse. Instead, non-soap cleansers and rinse carefully.
Pat rather than rub your skin dry, ensure your hands are completely dry and apply a moisturiser immediately after you wash your hands.
Hand cream for eczema
During eczema flare-ups you can use Eucerin AtoControl Acute Care Cream as an adjunctive hand cream for dermatitis, alongside medical treatment as recommended by your doctor. Adjunctive care is the medical term for a product that increases the benefits of another product.
This cream for eczema on hands contains Menthoxypropandiol (an extract of menthol) and Decanediol (an antibacterial active) which are proven to cool and calm skin and bring quick relief. Read more in Identifying and managing flare-ups.
Avoid triggers of hand dermatitis
Treatment can control atopic eczema on hands, but does not cure it. Identifying triggers early on can prevent long-term issues. The best treatment for hand eczema is to try and avoid whatever is triggering it. Here are some of the things that others have found can make a difference:
- Minimise contact with irritants - even water.
- Wear protective gloves at work and at home when in contact with water or chemicals.
- If you have to work for longer periods of time, wear cotton gloves under heavy duty vinyl or neoprene gloves. This protects skin from rubbing and prevents moisture build up inside the gloves.
- Dry the inside of rubber gloves after use and keep cotton gloves clean (wash them regularly using a fragrance- and soap-free detergent or your hand wash).
- Do not wash dishes or clothes by hand. Use a dishwasher or washing machine.
- Limit the amount of jewellery you wear, remove it at night and clean it regularly.
- Use disposable gloves if you work with foods such as onions, potatoes, meat or acidic fruits, and throw them away when you’re finished.
- Shampoo your hair while wearing protective gloves (waterproof vinyl with cotton liners), using rubber bands to prevent water getting into the gloves. Alternatively, ask someone else to wash your hair for you.
Medical treatment for dermatitis on hands
Topical steroids are the most common medical treatment option, as they reduce inflammation and relieve symptoms. Mild steroid creams and ointments (such as a 1% hydrocortisone) do not always address symptoms on thick skin so, in some cases, your doctor may recommend a stronger formulation.
These are usually applied twice a day, but overuse can lead to skin thinning. Stronger topical steroids may be required for eczema on the backs of hands or palms. Ultraviolet (UV) therapy is also sometimes used to treat severe hand dermatitis. If symptoms persist consult your doctor.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.