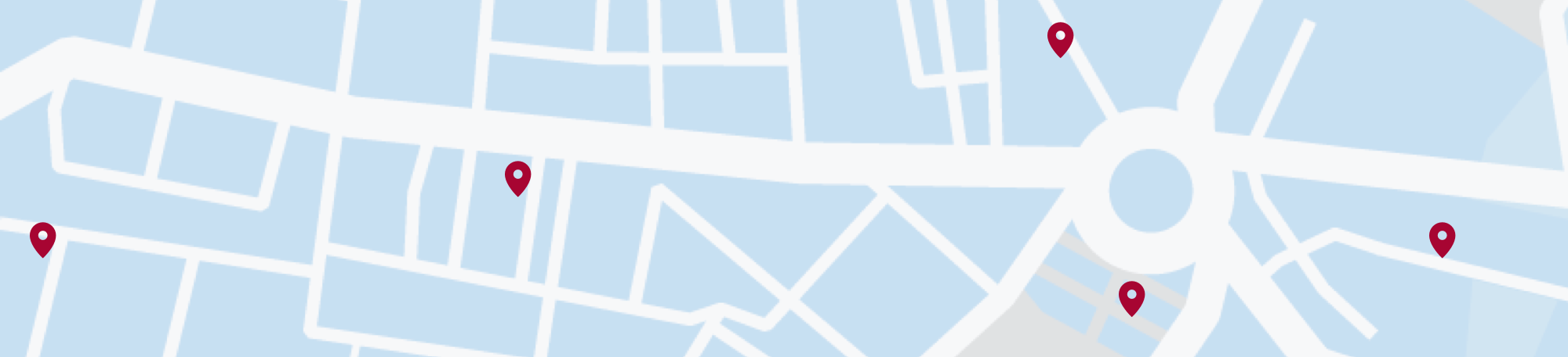
Atopic dermatitis, also known as atopic eczema, often flares up on the face; this is commonly known as facial eczema or facial dermatitis. Eczema can be uncomfortable anywhere on the body, but dermatitis on the face is particularly painful and debilitating due to sensitivity of facial skin.
This article explains how to recognise the symptoms of facial eczema and looks at the possible causes and triggers. It offers suggestions on how to care for atopic skin on a daily basis, as well as advice on how to soothe and calm your skin during flare-ups.
What is eczema on the face?
Face eczema is distressful precisely because it is so visible. Whilst non-contagious, it can create mental health issues for both children and adults, contributing to feelings of low self-esteem. It is known to have a considerable impact on the quality of life of those who suffer from it and their families. Read more about this in how atopic dermatitis affects sleep and quality of life.
Adult facial eczema can appear on the scalp, forehead and cheeks, behind the ears and in the delicate area around the eyes.
What causes dermatitis on the face?

Atopic dermatitis is a genetic disease that is linked to compromised skin barrier function and an immune disorder. Triggers vary from person to person but can include climate and pollution, stress or sensitivity to allergens like dust. There are also different types of eczema, which can determine different causes and treatments.
Other external aggressors include harsh facial cleansers, household products like soap or synthetic fibres, and certain make-up products. One person's eczema could be triggered by a fragranced product, but the same product may not cause a reaction for somebody else. This is why it’s important to speak to a doctor about your facial eczema.
The symptoms of atopic dermatitis are also its triggers. When your face feels itchy, it is very tempting to scratch it. This causes a bacteria called staphylococcus aureus to multiply and infect the skin, and this infection causes inflammation and itching, which worsens the condition. This vicious cycle is known as the ‘Atopic Skin Cycle’; you can find out more about it in Understanding Atopic Dermatitis.
What are the symptoms of dermatitis on the face?
Facial eczema can develop on its own, or with more widespread atopic dermatitis on the body. The symptoms of facial eczema are similar to those of atopic dermatitis in other areas:
- Skin becomes dry, itchy and irritable
- Redness/blotchiness
- Small, rough bumps
- Flakes (yellow flakes could indicate seborrheic dermatitis)
- Stinging or burning sensation
- Crusty blisters that can weep
- Bleeding (in severe cases)
If you notice dry patches on the face, you could be suffering from dry facial skin but not eczema. Unlike the tightness or mild flaking associated with dry skin, facial eczema usually involves cracked skin and severe itchiness. Scratching the itch only makes symptoms worse, and the damaged skin can become darker, infected and start to thicken.
How to get rid of eczema on the face
There is no known cure for atopic dermatitis, but there are steps that you can take to reduce flare-ups, both in terms of their number and severity. There are also ways in which you can prolong the periods between flare-ups and calm and soothe your skin during a flare-up.
Effective treatment requires an accurate diagnosis of your symptoms to check that you or your child do actually have atopic dermatitis, rather than one of the other kinds of facial dermatitis. You can learn more about the other types of eczema. By being aware of the type of eczema you have, you can provide the right treatment for it. Consult your doctor for advice and recommendations on the most appropriate treatments for your skin. Identifying any potential triggers and taking steps to avoid them is a key step towards reducing flare-ups.
Eczema on face treatment
Facial dermatitis requires careful treatment as the skin on our face can be irritated easily and is vulnerable to the side effects of topical therapy.
When caring for atopic facial skin on a daily basis, the primary aim is to prolong the non-acute phase, and regular moisturisation is crucial here. Look out for moisturisers (also known as emollients) that contain proven ingredients, such as:
- Licochalcone A: soothes skin and reduces redness
- Ceramides: strengthens the skin’s barrier function
- Omega-3 and Omega-6: soothes and nourishes the skin, while replenishing its protective barrier.
These are the key ingredients in Eucerin AtoControl Face Care Cream, which is proven to give atopic skin the daily care that it needs for an eczema on the face treatment. This cream can also be used during a flare-up, but you may find that your face needs additional care in order to relieve itching and soothe redness and irritation.
Eucerin AtoControl Acute Care Cream (with antibacterial Decanediol and cooling Menthoxypropandiol) has been specially formulated to give skin the care and comfort that it needs during flare-ups.
Both products can be used as an eczema cream for the face, alongside medical treatments which often help to calm severe symptoms. Find out more about them in Identifying and managing flare-ups.
There are several other steps you can take to care for eczema on the face:
- Gentle cleansing: Harsh cleansers and soap can exacerbate eczema on the face, so choose a mild facial cleanser such as Eucerin DermatoClean Refreshing Cleansing Gel. If you would like to rinse your cleanser off with water, use lukewarm water instead of hot water. Hot showers can cause further dryness and trigger facial eczema in some people. Pat gently with a soft towel to dry the skin instead of rubbing.
- Make-up: Choose products that are fragrance-free and, ideally, that have been proven to be suitable for sensitive skin. Applying make-up over a facial eczema rash can sometimes cause further irritation. Liquid foundations should be used instead of oil-absorbing powders, which can increase existing dryness. Be sure to remove your make-up fully before you go to bed.
- Sun protection: Some people find that a little sun helps with their symptoms, while others find that it exacerbates them. Either way, make sure you give your skin the protection it needs with products that are proven to be suitable for atopic facial skin. Read more about the importance of sun protection.
Medical treatment for dermatitis on the face
On the whole, treatment for facial dermatitis involves avoiding further irritation from triggers, switching to a gentle skin cleansing routine and treatment with medical products. Mild facial eczema can sometimes be treated with consistent moisturising and the skincare practices mentioned in this article. However, in many cases topical treatments are required.
Topical corticosteroids: Steroid creams are a key method of getting rid of the eczema on the face because they ease red, itchy skin. If recommended by your doctor, 1% hydrocortisone creams are preferred, as they post less risk of skin thinning. For this reason, they’re recommended for a short amount of time only (less than a month).
Topical calcineurin inhibitors: TCIs might be prescribed to treat facial eczema instead. The non-steroidal medications block chemicals that can make your eczema flare-up. These creams and ointments do not lead to skin thinning, so are commonly used for eczema on the face, including around the eyes and on the eyelids.
Ultraviolet phototherapy: This may be recommended for moderate to severe facial eczema if cream medications haven't treated the condition.
Facial eczema in babies and children
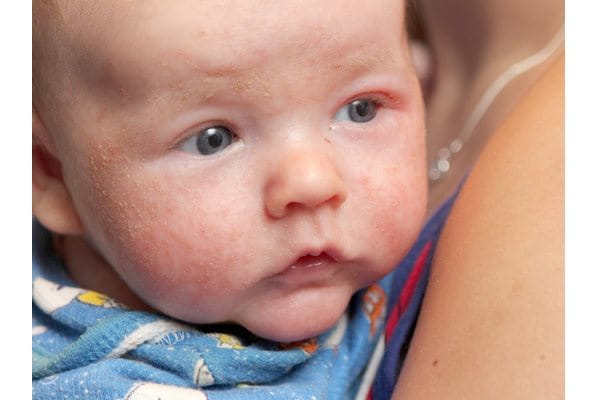
Facial atopic dermatitis, as with all forms of atopic dermatitis, is particularly common in babies and children and normally appears when they are between two and six months old. Eczema on the forehead and cheeks often appears first, but dermatitis on the face can spread to other parts of the body as they get older. Read more in Atopic dermatitis and babies and Atopic dermatitis and children.
Many children grow out of the condition. However, it can persist into adulthood and some adults suffer from dermatitis on the face without having had it in their youth. Some individuals only suffer from facial eczema for a week or two, but it can become a long-term condition for others.
Symptoms differ from person to person, from season to season, and even from day to day. The disease has two distinct phases: the flare-up, or acute phase, when the skin is at its most itchy and irritable, and the calmer period between flare-ups.
Other forms of facial dermatitis
Atopic dermatitis is not the only kind of eczema that can affect you or your child on the face. Other varieties include:
- Seborrheic dermatitis: Though the symptoms are similar, the skin is rarely itchy. This normally occurs around the hairline, ears, eyebrows and nose.
- Contact dermatitis: An allergic reaction to something with which your face comes into contact, such as make-up (although make-up may also trigger the symptoms of atopic dermatitis on the face). This often occurs around the hairline and eyes, as well as areas that come in contact with jewellery or perfumes like the earlobes and the neck.
- Photodermatitis: This occurs when the skin reacts to the sun. Sunlight can also be a trigger for atopic dermatitis, while other sufferers find that it can ease the symptoms.
Eczema on the neck
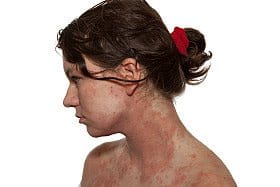
The neck can be compared to a set of skin folds, making it one of the most common areas affected by atopic dermatitis in childhood. During adulthood, 'head and neck dermatitis' is a specific form of eczema located on the neck and the face.
Though a small region, the neck is exposed to a number of triggers that can cause irritation, such as tight-necked clothes, jewellery and woolly scarves. Wearing cotton or fleece scarves and looser clothing can reduce tenderness. The neck is an easily accessible area, so eczema sufferers can sometimes scratch their neck without realising.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.

We work together with leading dermatologist and pharmacist partners around the world to create innovative and effective skincare products they can trust and recommend.












.jpg?rx=536&ry=0&rw=5616&rh=3763&hash=C8358E6898143DC9AA19E93A076F1DA2)