Published: October 2017
Last reviewed: November 2024
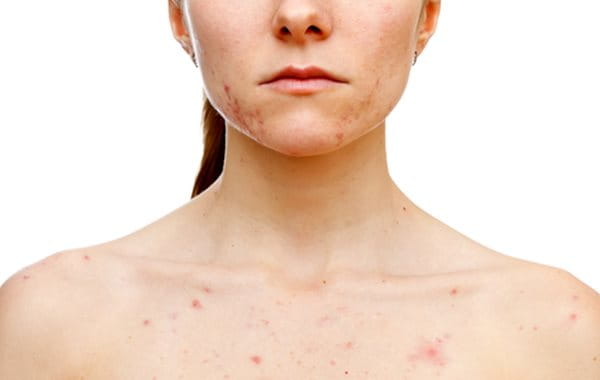
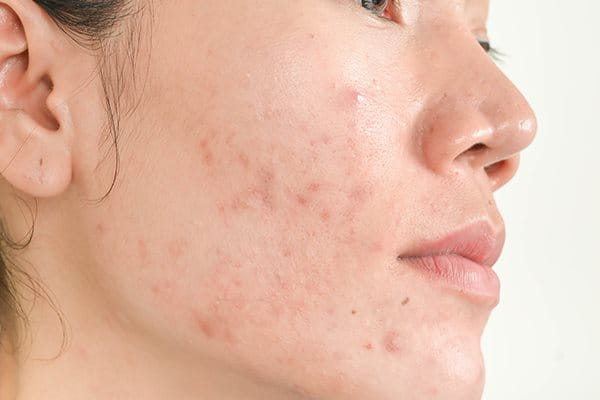
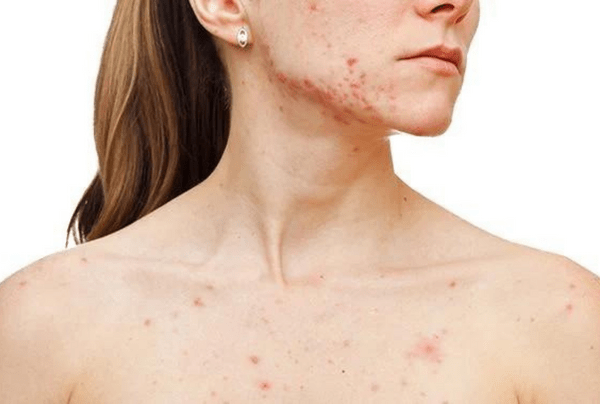
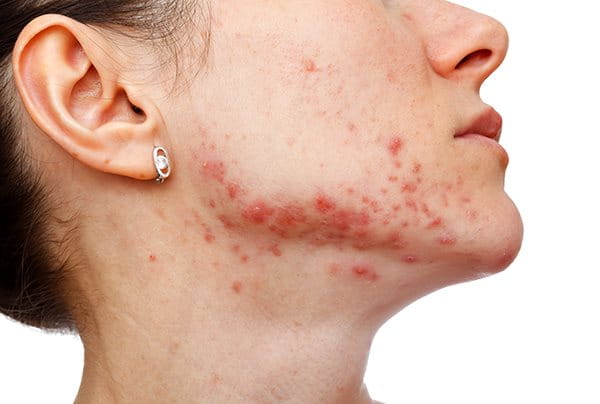
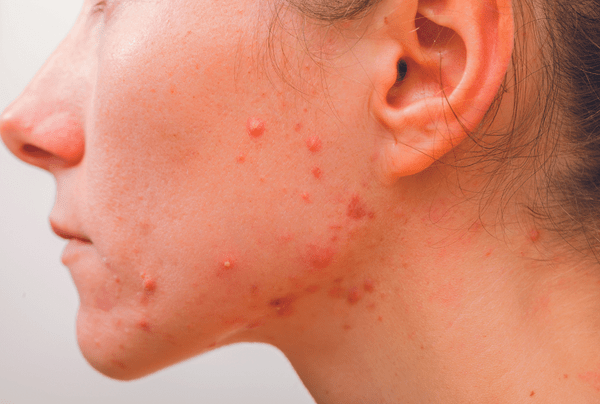
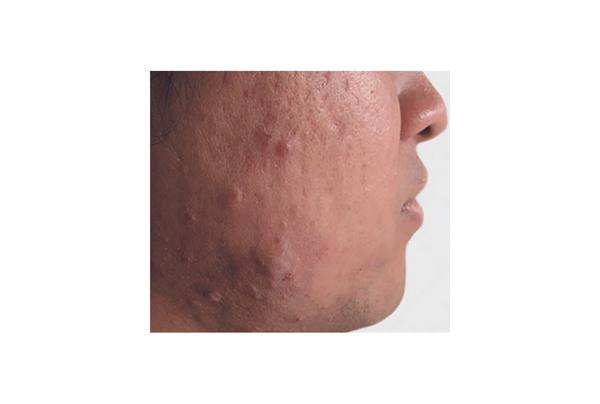
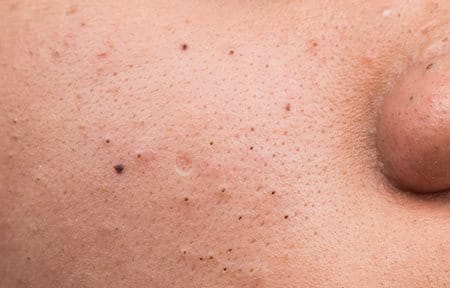
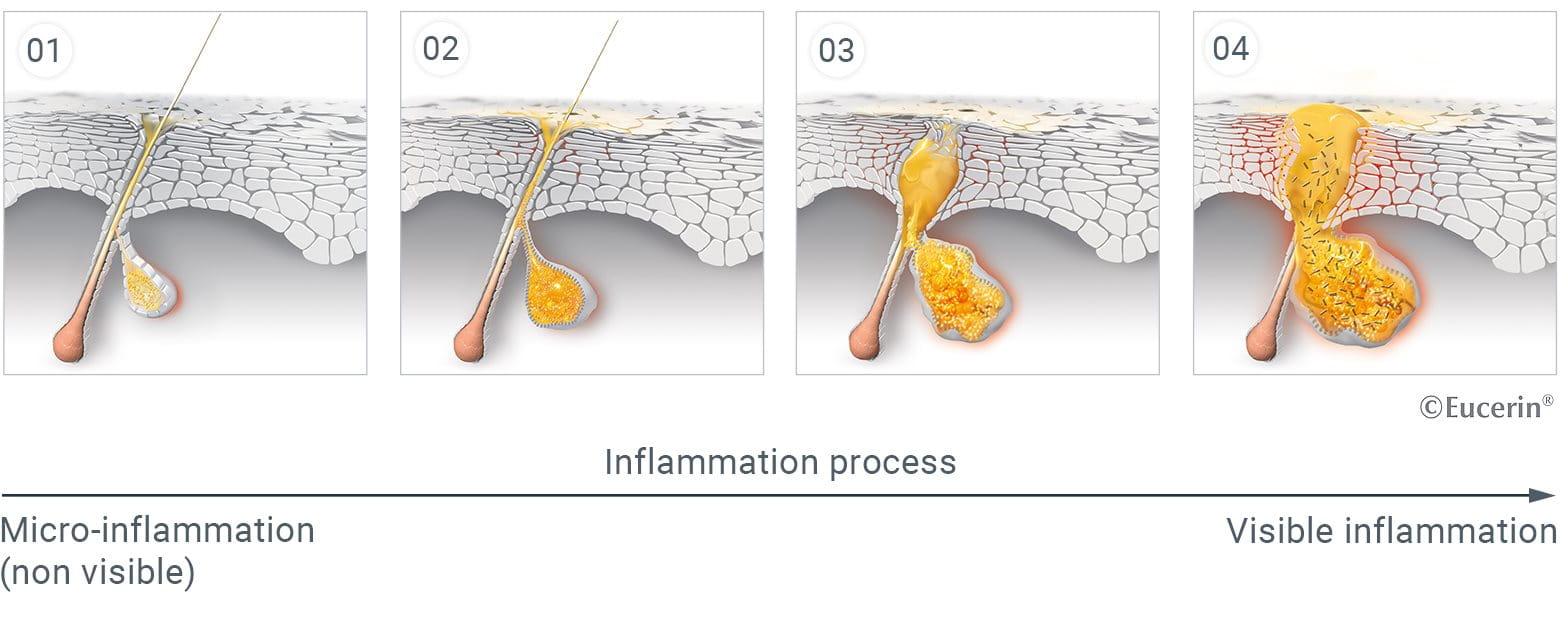
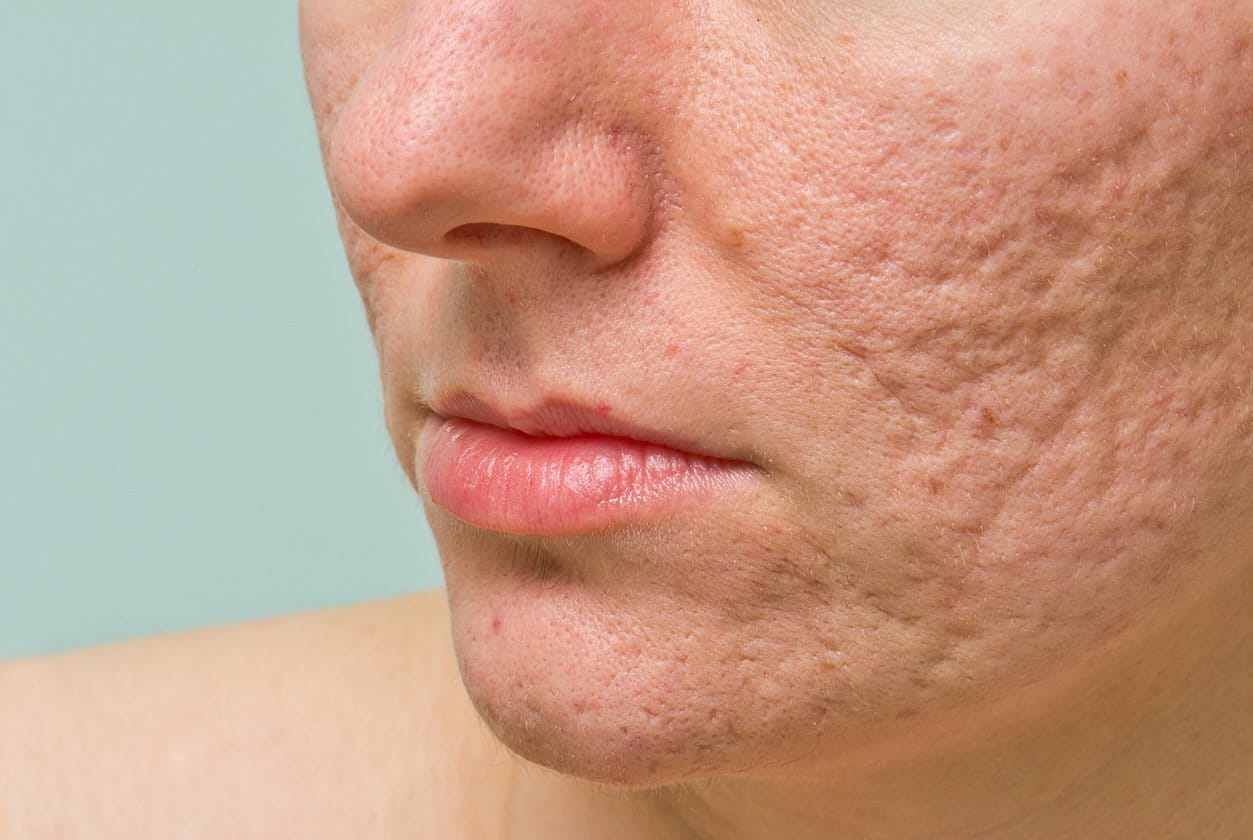
Dealing with acne-prone skin can be a frustrating and ongoing challenge for many people. Whether you experience occasional breakouts or frequent flare-ups, understanding your skin type and the best ways to care for it is key to achieving a clearer complexion.
In this article, we’ll explore the difference between blemish-prone and acne-prone skin, common triggers that can worsen it, and practical tips and treatments to help manage and improve your skin’s health. With the right approach, you can reduce breakouts and feel more confident in your skin daily.